Shin splints (Medial tibial syndrome)
What is shin splints?
One of the most common problems to affect the athlete, shin splints is thankfully one of the easiest conditions to treat. The term ‘shin splints’ is perhaps a little misleading as it 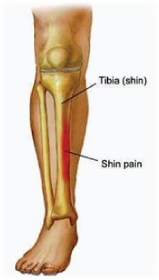 implies splintering of the bone or perhaps that sharp ‘splinters’ of pain should be felt. This is not the case. Patients with shin splints will complain of pain along the inner border of the shin (usually in the lower one-half or one-third of the bone) which worsens with running or repetitive, ballistic sporting activity such as football, basketball or netball. Pain steadily increases with activity and resolves with rest (though tenderness along the bone may persist for several days or even weeks after activity).
implies splintering of the bone or perhaps that sharp ‘splinters’ of pain should be felt. This is not the case. Patients with shin splints will complain of pain along the inner border of the shin (usually in the lower one-half or one-third of the bone) which worsens with running or repetitive, ballistic sporting activity such as football, basketball or netball. Pain steadily increases with activity and resolves with rest (though tenderness along the bone may persist for several days or even weeks after activity).
The major difficulty in treating shin splints is overcome by ensuring an accurate diagnosis. The pain of shin splints can mimic numerous other pathologies all of which require quite differing treatments. These pathologies include: tibial stress fractures, chronic compartment syndrome and tibialis posterior tendonitis to name a few. A thorough history and examination is usually all that is required to formulate a diagnosis and seldom is radiographic imaging required (x-rays, bones scans or nerve conduction studies may be suggested to exclude other diagnoses).
What causes shin splints?
It is thought that shin splints is primarily an overuse injury. This means that muscles (and tendons) on the inner part of the shin are required to work excessively and a local inflammatory reaction results. This overuse may be due to several causes:
- Poor biomechanics of the foot (pronation through the midfoot is common) causing muscles to work excessively during running
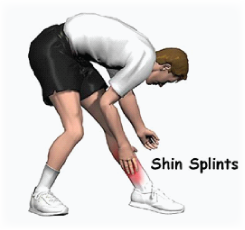 Poor footwear resulting in poor shock absorption or poor control of the foot during ‘strike’ and ‘stance’ phases of running. (Note – poor shock absorption alone is seldom the reason for shin splints despite some patients getting very good relief from improving the shock absorption in their footwear. It is thought that improved rear and midfoot shock control acts to decelerate the pronation of the foot and reduce eccentric workload of the tibial muscles)
Poor footwear resulting in poor shock absorption or poor control of the foot during ‘strike’ and ‘stance’ phases of running. (Note – poor shock absorption alone is seldom the reason for shin splints despite some patients getting very good relief from improving the shock absorption in their footwear. It is thought that improved rear and midfoot shock control acts to decelerate the pronation of the foot and reduce eccentric workload of the tibial muscles)- Running biomechanics. The way in which people run can contribute to excessive work of the medial tibial muscles. This needs to be corrected by a physiotherapist or exercise physiologist who is experienced with the causative sport. Over-striding and heavy heel strike are common culprits and, like all chronic biomechanical conditions, need to be evaluated by trained personnel and re-educated through repetition and dedication.
How will physiotherapy treat shin splints?
Your physiotherapist will take a detailed history of your problem and examine your legs closely to ensure an accurate diagnosis. Your physiotherapist may recommend orthotics 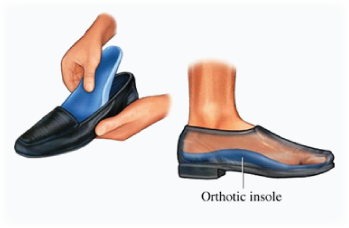 (inserts worn on the inside the shoe to correct biomechanical errors of the foot) or a period of taping to support the arch of the foot and reduce the workload of the shin muscles (you will be taught how to apply this taping to yourself when you play sport). You will also be shown how to massage the shin – a simple technique which can provide immediate short-term relief and can be used before and during sporting participation. You will be shown how to tape the shin or you may wish to invest in a shin brace – these are inexpensive and can be readily applied and removed without the painful loss of hair that comes with taping.
(inserts worn on the inside the shoe to correct biomechanical errors of the foot) or a period of taping to support the arch of the foot and reduce the workload of the shin muscles (you will be taught how to apply this taping to yourself when you play sport). You will also be shown how to massage the shin – a simple technique which can provide immediate short-term relief and can be used before and during sporting participation. You will be shown how to tape the shin or you may wish to invest in a shin brace – these are inexpensive and can be readily applied and removed without the painful loss of hair that comes with taping.
Your physiotherapist may also advise you on the appropriate footwear for your sport. The staff at Kingsley Physiotherapy will not recommend a particular brand of footwear and nor will they suggest a preferred retail outlet. Instead they will direct you toward the qualities you need to assess in a shoe.
Finally your physiotherapist may prescribe exercises to strengthen the muscles around your shin. These are very specific exercises that aim to correct the workload distribution between the small muscles of your calf. The reality is however, that there is not a lot of research data supporting the benefit of these strengthening programmes. What evidence there is, suggests patients need to be dedicated to a lengthy (3 to 6 month) programme of daily exercises under close supervision and gradual progression by a physiotherapist or exercise physiologist. This is a lengthy and expensive process. Your physiotherapist will discuss other medical options to assist your recovery that are quicker and cheaper.
If you have any further questions on this subject, or you would like to contact the physiotherapist best suited to managing your problem please call or email us.
© Andrew Thompson