Osteoarthritis
Definition:
Osteoarthris (OA) is a common cause of joint pain and stiffness. It is characterized by the progressive degeneration of joint cartilage. OA is the most common form of arthritis typically affecting people beyond the age of 45. Unlike inflammatory arthropathic diseases such as rheumatoid arthritis or psoriatic arthritis, OA is not systemic illness – it only affects the joint(s). It is caused by the gradual destruction of hyaline cartilage that ‘lines’ the bone ends in a joint. That being said, to think of OA as a simple ‘wear-and-tear’ process is to overlook the complexity of this pathology. OA must also be considered in the context of the body’s ‘failure’ to repair and recover from damage to joint cartilage. To this end it can be influenced by numerous factors including: smoking, hydration, body weight, diabetes, alcohol consumption, prior joint trauma or surgery, genetic predisposition, liver function and numerous other variables.
Symptoms:
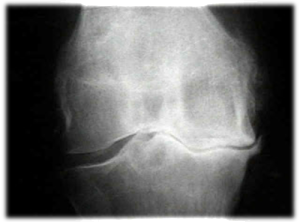 The weight bearing joints of the lumbar spine and lower limb are most commonly affected although any joint has the potential to develop OA. Symptoms include pain and stiffness, crepitus (creaking/cracking joints), inflammation and swelling (although this is often minor or even absent), weakness and a loss of joint range (either due to pain or mechanical restriction). In the early stages pain and stiffness is experienced during particular activities (ex. kneeling, climbing stairs, walking up hill) but over time the degeneration can progress to the point that pain is experienced at rest independent and requires less and less physical provocation.
The weight bearing joints of the lumbar spine and lower limb are most commonly affected although any joint has the potential to develop OA. Symptoms include pain and stiffness, crepitus (creaking/cracking joints), inflammation and swelling (although this is often minor or even absent), weakness and a loss of joint range (either due to pain or mechanical restriction). In the early stages pain and stiffness is experienced during particular activities (ex. kneeling, climbing stairs, walking up hill) but over time the degeneration can progress to the point that pain is experienced at rest independent and requires less and less physical provocation.
Joint stiffness is most notable after periods of rest or immobility (first thing in the morning or after prolonged recumbence). Pain and stiffness may be eased with movement and by the application of heat.
Diagnosis:
The diagnosis of OA is usually made clinically. A detailed history will reveal the slow development of pain and stiffness in the absence of any notable recent trauma or injury. There is often tenderness along the joint margin though unlike arthropathies such as gout or rheumatoid arthritis there is seldom any appreciable warmth, redness or swelling. There may be bony irregularity of the joint margins and deformity of the limb.
X-rays may reveal joint ‘narrowing’, osetophytic lipping, and bony deformity. Examination of the effected limb may reveal an asymmetrical appearance (compared to the opposite limb). Such findings in the absence of recent trauma/injury when combined with other predisposing factors (outlined below) make the diagnosis of OA highly likely.
Factors which confer an increased likelihood of OA include: age (over 40), raised body-mass-index (obesity), smoking, long term alcohol consumption, diabetes, prior joint injury or surgery, a family history of OA, Heberdens/ Bouchards nodes and other joint pathologies – OA may co-exist with other forms of arthritis.
X-rays are the most cost-effective means of diagnosing OA but often CT or MR imaging can help to exclude other soft tissue pathologies that may cloud the clinical picture.
Treatment:
Symptom management as well as joint maintenance and preservation are key to treating an osteoarthritic joint. Some fundamental principles should be addressed with all patients:
- Cease smoking
- Reduce body weight
- Reduce alcohol intake
- Maintain water intake
- Listen to your body – OA sufferers will experience periods of symptom exacerbation (increased pain) and remission (reduced pain and improved function). During remissions it is vital to exercise and mobilise the joint. Exacerbations can be managed with rest, analgesia, physiotherapy and corticosteroid injections.
Physiotherapy treatment:
Your physiotherapist will confirm the diagnosis of OA and exclude or manage other co-existing joint pathologies. Treatment may include: joint mobilisation or manipulation, strengthening or weight loss exercises, muscle release techniques, ergonomic assessment, postural and biomechanical correction, joint taping or bracing, orthotic prescription and hydrotherapy or gym-based exercise programmes.
Ultrasound, laser and interferential treatments have no value in the treatment of OA.
Medical treatment:
In the in early stages of OA simple interventions are usually sufficient to reduce pain: rest, heat application, paracetamol, non-steroidal anti-inflammatories or other oral analgesics. Failing this, corticosteroid joint injections may be advised. Synvisc® is a gel-like product (hyaluronic acid) which can be injected into mild to moderately arthritic joints. The benefit that Synvisc® may infer is almost always outweighed by its exorbitant cost and hence other treatment options are generally pursued.
Corticosteroid injections can provide substantial and prolonged relief. For optimal results steroid injections should be combined with appropriate joint bracing/taping and physiotherapy-based rehabilitation. Corticosteroid injections can achieve very good results in the short to medium-term…. unless: the diagnosis is inaccurate or incomplete, when the injection has been inaccurately placed, when the patient has not followed appropriate after-care advice or when injections are given in a ‘last-ditch-effort’ to avoid surgery.
Prolotherapy treatment:
Prolotherapy describes a variety of treatments which aim to “proliferate” damaged tissue or ‘re-ignite’ the inflammatory-repair process within a joint or extra-capsular soft tissue (tendon, bursa, fascia etc). Mild to moderate OA (in the absence of other intrarticular joint pathologies) is best treated with Platelet Rich Plasma (PRP). Results will take 2 to 3 months and treatment costs around $350 in total.
Surgical treatment:
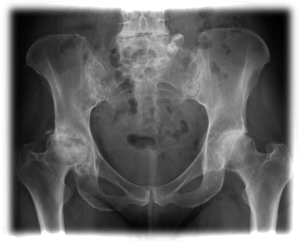 Surgical treatments for OA are relatively limited. They are confined to:
Surgical treatments for OA are relatively limited. They are confined to:
- Arthroscopic debridement of the joint
- Joint realignment surgery
- Joint replacement surgery
- Joint fusion
Such surgeries can be very successful in restoring function and reducing pain. Most surgeries require well timed and appropriately progressed rehabilitation. The physiotherapists at Kingsley Physiotherapy can assist you with this and are well suited to advising on appropriate medical or prolotherapy interventions.
If you have any further questions on this subject, or you would like to contact the physiotherapist best suited to managing your problem please call or email us.
© Mr Blake McConville and Dr Andrew Thompson