Osteitis Pubis
What is osteitis pubis?
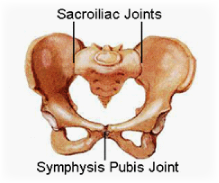
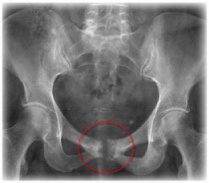
Osteitis pubis is an inflammation of the symphysis pubis – the cartilage based joint between the left and right pubic bones (pictured right). It is most commonly seen in sports where jumping, kicking and running are required. For this reason, Australian rules football provides an ideal climate for this type of overuse injury. If left untreated, it may lead to sclerosis (roughening), separation or displacement of the pubic junction (x-ray image below) and can spell disaster for the career of an athlete.
Numerous factors may lead to the development of osteitis pubis. Alterations in the type of exercise regime undertaken (intensified training, running on hard or uneven surfaces or returning to sport after a period of relative rest) as well as biomechanical factors (poorly fitted/ worn shoes or intrinsic disturbances of gait, running and lower limb biomechanics) may provide they key to determining the cause of this condition. Leg length discrepancies are frequently cited as a cause of osteitis pubis though in reality this accounts for a very small portion of presentations. Be cautious of investing in expensive orthotics or footwear in order to treat this condition.
What are the symptoms of osteitis pubis?
Typically osteitis pubis presents as a gradual development of pain in the groin. Patients will describe this pain as an ache or occasionally as a sharp “grabbing”. They may experience symptoms either centrally or to one side. Commonly they will describe specific activities that aggravate their symptoms such as kicking, running or jumping. In severe and progressive cases, this pain may be elicited by simple daily tasks – getting in and out of a car, dressing or even walking.
Osteitis pubis following pregnancy (and vaginal child birth) is also common and this often proves the most challenging presentation to treat conservatively.
The physiotherapy assessment of osteitis pubis
Your physiotherapist will take a detailed history of your symptoms. For female patients this history will include questions regarding possible gynaecological presentations which may cause groin pain – cystitis, endometriosis, urethritis or pelvic inflammatory disorders to name a few. Your physiotherapist will then undertake a thorough examination of the lower back, hip, sacroiliac joints and symphysis pubis. There are numerous conditions that can mimic the symptoms of osteitis pubis and it is important that the more sinister of these be excluded. You will also be examined for inguinal, femoral and umbilical herniations as a potential source of your pain.
The physiotherapy treatment of osteitis pubis
The role of physiotherapy in the treatment of osteitis pubis is essentially a defensive strategy – a means of damage control. Exercises to strengthen or stretch muscles around the pelvis in order to achieve greater stability and muscle balance are frequently met with significant compliance issues – the exercises are tedious, boring and take several months to have any observable effect on the patient’s ability to return to his or her chosen sport. More definitively the role of physiotherapy is three fold:
- To accurately diagnose the condition (and in so doing, exclude other more readily treatable pathologies)
- Educate the patient in order to prevent reoccurrence or progression of symptoms. This will involve the prescription of exercises as well as sport-specific training and biomechanical advice.
- Outline the various medical and surgical treatment options for osteitis pubis
Abstaining from sport is essential if conservative management is to have any effect. This usually requires at least 4 to 6 weeks of complete rest from high impact activities (swimming and cycling may be continued). A short course of non-steroidal anti-inflammatory medication may also help with the acute pain but will not shorten the recovery time. It is during this ‘rest period’ that strengthening and stretching exercises need to be carried out with feverish diligence. These exercise programmes need to be specified for the individual (their body type, strength, flexibility and the sport they play) but usually involve stretching of the hip flexors and groin muscles and strengthening of the gluteus medius and transverses abdominus muscles. There is little evidence to support the strengthening of the pelvic floor musculature although this may still be included in order to facilitate co-contraction of the deep abdominal musculature (and because it has numerous other benefits for both men and woman).
Following this period of rest, your physiotherapist will draft a graduated return-to-sport programme. Usually another 4 to 6 weeks of progressive exercises are needed to reintroduce the patient to normal sporting activities. Physiotherapy is most certainly not the magic bullet most patients are seeking for the management of osteitis pubis.
Your physiotherapist may also provide you with a compressive brace. This is a simple strap that fits around the lower waist and compresses the pelvis. This is perhaps most effective in cases of marked instability at the symphysis pubis as may be seen following child birth or pelvic trauma.
If there is doubt about the diagnosis of osteitis pubis, your physiotherapist may recommend a bone scan. This imaging technique will show areas of high cellular turnover in the body as is seen at fracture sites or areas of skeletal inflammation. Plain film x-rays may not show any sclerotic change (especially in the early stages) and can be misleading of the diagnosis. Occasionally, single leg standing x-rays (stork views) may show positional change between the left and right pubic bones but again this is not a reliable test and does not alter the overall management of the condition.
The medical management of osteitis pubis
In the acute stage, osteitis pubis can be managed with a well positioned corticosteroid injection. This can provide immediate and substantial relief of pain but does not address the long term management of the condition. This option may be appropriate if work or sporting commitments demand a quick, short-term fix. Ideally this approach should be followed up with advice on exercise and a slow, progressive return to sport.
A better long term management option is prolotherapy – the injection of an irritant (usually a simple sugar solution or the patient’s own blood) into the ligaments that support the pubic symphysis in order to encourage proliferation of ligament tissue (a fibroblastic response) and stabilise the region to movement. This involves between 3 to 5 injections into the region (usually carried out at least 1 to 2 weeks apart). It is a technique that needs to be performed by an experienced (and preferably an empathetic) doctor. When successful, patients will return to normal sporting activities in 2 to 4 months. This approach generally negates the need for a specific exercise regime and does away with the cost associated with physiotherapy consultations. Most physiotherapists will happily talk you through your ‘return-to-sport’ programme over the telephone or via email.
If you have any further questions on this subject, or you would like to contact the physiotherapist best suited to managing your problem please call or email us.
© Andrew Thompson