Groin pain
The groin region is defined as that part of the inner and upper thigh where the pelvis 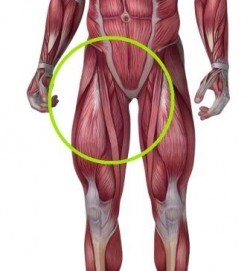 “meets” the lower limb. More specifically it refers to several muscles and tendons of the thigh that are collectively referred to as the ‘adductors’. In practice, pain in the region of the groin can arise from numerous local tissues (bones, ligaments, cartilage, tendons and muscles) and may also be a site of pain referred from other tissues within the pelvis, the lumbar spine, the sacroiliac joint or the knee.
“meets” the lower limb. More specifically it refers to several muscles and tendons of the thigh that are collectively referred to as the ‘adductors’. In practice, pain in the region of the groin can arise from numerous local tissues (bones, ligaments, cartilage, tendons and muscles) and may also be a site of pain referred from other tissues within the pelvis, the lumbar spine, the sacroiliac joint or the knee.
Groin pain is a common presentation in the sporting population and a thorough understanding of lumbar, pelvic, visceral and lower limb anatomy is vital to accurately diagnose a patient with groin pain. A physiotherapist requires extensive knowledge in anatomy, physiology, biomechanics and pharmacology to successfully manage such patients.
The ‘groin patient’ poses some interesting and unique challenges to the experienced physiotherapist. Anatomically the groin region includes the muscles of the lower abdomen, muscles of the thigh, gluteals and pelvic floor, the abdominal organs (viscera), the inguinal canal and its contents, the femur, the pubic, iliac and ischial bones of the pelvis, the pubic symphysis, the hip adductor muscles (the true ‘groin’ muscles), pelvic organs (lower colon, bladder, uterus, ovaries and vagina) and the external genitalia. Additionally, groin pain may also arise from the lumbar spine, hip joint and the sacroiliac joint. One can now begin to understand the complexity of treating the ‘groin patient’.
Causes of groin pain
The hip joint and muscles of the groin are placed under enormous strain during weight-bearing activity. This is augmented in sports that require rapid change of direction, frequent acceleration and kicking. Australian rules football, rugby and netball lend themselves wonderfully to a physiotherapist’s caseload.
Groin injuries may be acute (recent onset) or chronic (long standing). Very frequently they involve more than one pathology – often several sources of pain contribute to a persons symptoms. A skilled physiotherapist must dissect this complex jigsaw and utilise their manual, medical and exercise therapy skills to treat the patient. Unfortunately many physiotherapists shy-away from such ‘complicated’ patients and needless injections or surgery often ensue.
The potential causes of groin pain are daunting to consider. A physiotherapist will broadly stratify patients according to the likely ‘tissue’ source of their symptoms – tendons, muscles, nerves, ligaments, fascia, etc. They will then assess the biomechanical forces at play that have caused or are exacerbating the symptoms.
A physiotherapist will assess the biomechanics associated with a patient’s sporting or work activities as well as any postures or ergonomic stressors that may be contributing to the problem. Common exacerbating activities of groin pain include kicking, walking or running, squatting/lunging and standing after prolonged sitting.
It is also important for a physiotherapist to assess the numerous genetic and medical predisposing factors for groin pain. Elderly, diabetics, smokers, pregnant women, athletes, long-term corticosteroid users and the obese are all prone to developing groin pain. This is not a problem confronting athletes only.
Symptoms
Problems with the groin will usually cause focal symptoms –pain in the region of the primary pathology and, less commonly, local tenderness. Groin pathologies may also give rise to lumbar, abdominal, thigh and knee pain.
Additionally, groin pain may be associated with altered menstrual symptoms (dysmenorrhea, amenorrhea and menorrhagia), bowel changes (constipation, flatus or diarrhea), regional swelling (epididymo-orchitis, hernias) or skin changes (as seen in fungal groin infections, psoriasis and dermatitis). Your physiotherapist should also discuss the possibility of sexually transmitted infections such as gonorrhea and chlamydia.
Symptoms of groin pain arising from musculoskeletal sources may include:
- Pain following strenuous or unaccustomed activity. Pain in these cases is nearly always one sided (not central or bilateral).
- Loss of power when sprinting and kicking.
- A sensation of stiffness or tightness when standing after periods of rest (sitting or lying).
- Pain with coughing or sneezing and pain with contraction of the abdominal muscles (sit-ups)
- Pain or tightness when the thighs are separated (getting in or out of a car).
Physiotherapy Management
- Stretching and massaging the adductor muscles. In many cases of groin pain, releasing the hip flexors (iliopsoas, quadriceps and lower abdominal muscles) will also be advised.
- Strengthening the ‘core’ muscles – the abdominal, lower back and pelvic floor muscles. This can help “unload” the strain placed on the groin muscles and the hip joint.

- Releasing the tensile structures of the hip – ligaments and tendons.
- Braces and splints – your physiotherapist may recommend groin or lumbar braces to support the pelvis and sacroiliac joint.
- Rest – as with most inflammatory conditions the ‘groin patient’ may need to rest from those activities or postures that exacerbate their symptoms. This is not always easy or practical (especially when vocational activities are to blame) but when the surgical and medical options for managing groin pain are limited, rest can be a simple and worthy component of a full rehabilitation programme. Rest can be a masterful prescription.
There is no benefit to be gained by the use of ultrasound, interferential, laser or acupuncture. Research on these modalities has repeatedly proven their lack of efficacy.
Medical Management
- Non-steroidal anti-inflammatories and analgesics may assist with acute groin pain.
- Steroidal anti-inflammatories (cortisone) may be prescribed. These can be taken orally or applied topically. More commonly, cortisone injections to the regional tendons or joints will be prescribed.
- Platelet rich plasma (PRP) or Synvisc® injections into the hip joint may be recommended.
- Autologous blood injections (ABI) are a very promising adjunct to managing a multitude of chronic inflammatory and degenerative pathologies. Click here for more information.
- Extracorporeal shockwave therapy is used to treat chronic soft tissue inflammatory pathologies – bursitis, tendonoses. You may be referred to the doctors at Kingsley Medical if shockwave therapy is considered.
Surgical Management
Surgical options for treating the groin patient are limited. Hernia mesh repairs, tenodesis, arthroscopic hip surgery, tendon debridement, and hip replacement may be suitable.
To book your appointment at Kingsley Physiotherapy with the therapist best suited to treating your groin pain click here.
© Kingsley Physiotherapy – Ms Penny Stern and Dr Andrew Thompson