Carpal tunnel syndrome
What is carpal tunnel syndrome?
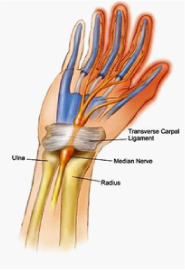 Carpal tunnel syndrome is by far the most common of the peripheral entrapment neuropathies – i.e. a neurological condition that occurs when one of the body’s nerves (in this case the median nerve) gets compressed somewhere along its pathway. The median nerve is an important nerve of the upper limb that runs through the front of the forearm and the middle of the wrist before branching off in the hand to supply the thumb and some of the fingers. As the median nerve passes over the wrist joint it traverses through a tightly packed opening formed between the small bones of the hand (the ‘carpals’) and a thick ligament on the palm of the hand. Swelling within this tunnel (discussed below) can compress the median nerve and result in pins and needles, numbness, itchiness or even weakness in the muscles of the hand and thumb.
Carpal tunnel syndrome is by far the most common of the peripheral entrapment neuropathies – i.e. a neurological condition that occurs when one of the body’s nerves (in this case the median nerve) gets compressed somewhere along its pathway. The median nerve is an important nerve of the upper limb that runs through the front of the forearm and the middle of the wrist before branching off in the hand to supply the thumb and some of the fingers. As the median nerve passes over the wrist joint it traverses through a tightly packed opening formed between the small bones of the hand (the ‘carpals’) and a thick ligament on the palm of the hand. Swelling within this tunnel (discussed below) can compress the median nerve and result in pins and needles, numbness, itchiness or even weakness in the muscles of the hand and thumb.
What are the symptoms of carpal tunnel syndrome?
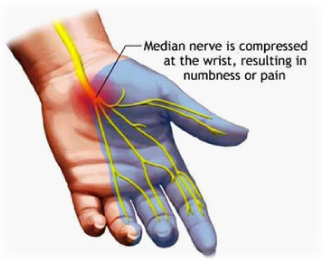 The symptoms of carpal tunnel syndrome generally develop over a period of time – usually weeks or months. Patients may describe typical neurological symptoms (symptoms indicative of nerve compromise) such as itching, burning, pins and needles and numbness in the thumb, index finger and middle finger. The symptoms may initially be experienced at night in one or both hands. Over time, such symptoms may then be experienced during the day and may lead to a feeling of weakness and the need to “shake out” the hand in order to obtain relief. In chronic cases, the muscles at the base of the thumb may show signs of wasting (the 1st and second lumbricals and the thenar eminence). The remaining small muscles of the hand are supplied by the ulna nerve and are hence spared in carpal tunnel syndrome. The ulna nerve is susceptible to compression at the elbow (a condition called ‘cubital tunnel syndrome’) and at the wrist (‘Guyons’s canal syndrome’). Compression of the ulna nerve produces similar symptoms but in a different location within the hand and may result in the classical “claw hand” appearance.
The symptoms of carpal tunnel syndrome generally develop over a period of time – usually weeks or months. Patients may describe typical neurological symptoms (symptoms indicative of nerve compromise) such as itching, burning, pins and needles and numbness in the thumb, index finger and middle finger. The symptoms may initially be experienced at night in one or both hands. Over time, such symptoms may then be experienced during the day and may lead to a feeling of weakness and the need to “shake out” the hand in order to obtain relief. In chronic cases, the muscles at the base of the thumb may show signs of wasting (the 1st and second lumbricals and the thenar eminence). The remaining small muscles of the hand are supplied by the ulna nerve and are hence spared in carpal tunnel syndrome. The ulna nerve is susceptible to compression at the elbow (a condition called ‘cubital tunnel syndrome’) and at the wrist (‘Guyons’s canal syndrome’). Compression of the ulna nerve produces similar symptoms but in a different location within the hand and may result in the classical “claw hand” appearance.
What causes carpal tunnel syndrome?
There are numerous factors which may contribute to the development of carpal tunnel syndrome. In most cases it is thought that sufferers have a genetic predisposition – that is, the carpal tunnel is physically smaller in some individuals and hence more susceptible to compression of the median nerve in the event of local or regional swelling. Factors which can precipitate swelling in this area include local trauma (work stress, use of mechanical and vibrating machinery) or systemic conditions such as hypothyroidism, menopause, pregnancy, diabetes, rheumatoid arthritis and pathologies relating to renal and pituitary dysfunction. In many cases, no obvious cause can be identified.
How is carpal tunnel syndrome diagnosed?
It is important to differentiate carpal tunnel syndrome from the numerous other pathologies that can give rise to similar symptoms in the hand. Your physiotherapist will perform a thorough history and physical examination to exclude local conditions such as, tenosynovitis, bursitis, tendonitis as well as other neuropathies and vasculopathies. The physiotherapist will also assess the elbow, shoulder and neck to exclude the referral of symptoms from these regions. X-rays may be considered to exclude pathologies such as rheumatoid arthritis, fractures or osteomyelitis whist blood tests may be suggested to assess for diabetes or thyroid dysfunction. Ultrasound imaging to assess the movement of the median nerve as the wrist is flexed and extended is now rarely used as it adds little to the diagnosis and nothing to the treatment plan.
If there is uncertainty about the diagnosis of carpal tunnel syndrome or in cases where surgical or semi-invasive treatment methods are being considered, nerve conductions studies and electromyography may be suggested. This involves assessing the electrical function of the nerve and muscles to ascertain if and where a nerve compression exists.
Treatment of carpal tunnel syndrome
It is always important to commence treatment as soon as possible. In the early stages of the condition, conservative interventions such as physiotherapy have a far better chance of eliciting results than in cases that have gone untreated for several months. Initially your physiotherapist will incorporate a series of manual release techniques aimed at loosening the soft tissue structures in the palm of the hand. Treatment will also focus on loosening the muscles of the forearm and a home stretching routine will be given to 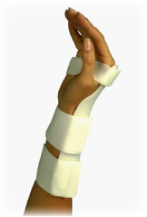 complement this. You may have your hand or wrist taped in one of several ways (depending on the chronicity and severity of symptoms). A carpal-compression taping is the simplest of these and in the first 4 to 6 weeks of the condition, may be sufficient to fully resolve the symptoms. The complexity of taping techniques tends to increase the longer that symptoms have been present. Often these taping techniques can be taught to the patient and this can reduce the cost of physiotherapy considerably.
complement this. You may have your hand or wrist taped in one of several ways (depending on the chronicity and severity of symptoms). A carpal-compression taping is the simplest of these and in the first 4 to 6 weeks of the condition, may be sufficient to fully resolve the symptoms. The complexity of taping techniques tends to increase the longer that symptoms have been present. Often these taping techniques can be taught to the patient and this can reduce the cost of physiotherapy considerably.
If your symptoms occur mainly at night, you may be advised to wear a wrist splint that supports the wrist in an extended position. If your symptoms are also present during the day or are aggravated by your work environment, splints can be chosen that allow for normal functioning of the fingers and thumb. There are numerous splints available for carpal tunnel syndrome and often this intervention alone can dramatically reduce or resolve the symptoms.
It is important that any underlying pathologies (diabetes, thyroid dysfunction etc) be treated concurrently. In some case, the medical management of these precipitating conditions will negate the need for physiotherapy intervention.
If you have any further questions on this subject, or you would like to contact the physiotherapist best suited to managing your problem please call or email us.